Brain and mental health from infancy to adolescence.
Research has shown that 75% of mental health problems emerge before the age of 24.
Experts at Oxford are analysing the brain’s development from infancy through to adolescence. They’re working to measure pain in babies and infants, and understand the psychological processes used in language.
Tags:


Our researchers are analysing the mental health of children and adolescents and investigating how COVID-19 impacted wellbeing.
They’re aiming to understanding depression, anxiety and eating disorders, and improve child and adolescent mental health services.
Infant neuroscience and developmental psychology.

Analysing the infant brain.
Oxford’s Paediatric Neuroimaging Group from the Department of Paediatrics brings together scientists, clinicians, and engineers to further our understanding of early human brain development.
The multidisciplinary group is led by Professor Rebeccah Slater, and it focuses on better understanding the development and treatment of infant pain, and understanding the impact of apnoea on the developing brain.
The group provides a unique research environment that integrates Oxford’s major children’s hospital and its staff with advanced medical imaging, clinical trials, neuroscience and ethics expertise.
Neonatal:
Relating to newborn children
The group aims to design high-quality, interdisciplinary neonatal research and clinical trials, share neonatal brain imaging data across disciplines, develop the next generation of academic clinicians and scientists, and enhance science communication and public engagement.
The group focuses their research on human neonatal brain development, developing new approaches to analyse data recorded from infants, including Magnetic Resonance Imaging (MRI), electroencephalographic (EEG), and physiological data.
They are also investigating whether changes in breathing affect brain development, and how the brain and respiratory systems mature in premature babies, assessing the efficacy of pain-relieving medications and non-pharmacological interventions, such as parental touch, and using MRI and EEG to investigate how the human brain changes in early development.
Measuring pain in infants and babies.
Infant pain has negative long-term consequences, and prevention is a clinical priority.
The Paediatric Neuroimaging Group aims to understand the mechanisms that drive and modulate pain perception in early human development, with the overarching goal of improving treatment of pain in all infants.
As recently as the 1980s, babies undergoing surgeries weren’t given any pain medication – instead being given a muscle relaxant to paralyse them while in the operating room.
Speaking to National Geographic, Dr Fiona Moultrie explains that ‘although there has been great progress, we still don't fully understand pain in neonates’.
Funded by Wellcome, the group’s work in this area investigates the impact of gentle touch on infant pain and how surgical procedures affect infant pain. They are identifying brain signatures and physiological markers of infant pain.
They are also investigating how early life infections impact pain perception in infants, with researchers, led by Dr Maria Cobo, discovering that infection can increase a baby’s sensitivity to pain, which may last longer than the infection.
One of the major challenges in assessing and managing pain in very young children is the child’s inability to communicate their feelings. Instead, paediatricians have needed to rely on observations of facial expressions or heart rates to see whether babies are experiencing pain.
Researchers, including Associate Professor Caroline Hartley, Professor Rebeccah Slater and colleagues from the University as well as the Great Ormond Street Hospital, developed a non-invasive way of measuring pain-related activities based on electroencephalographic (EEG) recordings of brain activity.
Cognitive development.
The Oxford University BabyLab works with children aged from six months to three years to study how infants learn to extract meaning from speech.
One of the first research facilities in the UK dedicated to infant research, the lab was founded in 1992 and is part of the University’s Department of Experimental Psychology.
Since inception, over 7,500 infants have taken part in the lab’s research, which aims to analyse how infants learn to recognise words, learn new words and concepts, and identify how to use words to talk about and represent the world.
BabyLab also collaborates with the University’s Language & Cognitive Development research group.
Led by Professor Kate Nation, the group is interested in various different aspects of psycholinguistics, with a particular focus on learning to read.
Psycholinguistics:
The field of study in which researchers investigate the psychological processes involved in the use of language
The group is the home of ReadOxford, where researchers have been investigating what eye movements can tell us about reading, and have developed a nationwide citizen science project for 5-16 year olds called Word Detective.
Both BabyLab and the Language & Cognitive Development research group form part of the Developmental Psychology research grouping within the Department of Experimental Psychology.
Researchers in this grouping are working closely with local schools, teachers, families, charities and therapists to investigate attentional processes, the causes and consequences of autism and alexithymia, and the development and evaluation of interventions for children with mathematical difficulties.
Experts are also aiming to understand the causes of children’s learning difficulties, developing interventions to help support them, and are using brain imaging and brain simulation to study speech perception and production.
Finally, the Risk & Resilience group, led by Professor Lucy Bowes, studies the interplay between biology and social context in child and adolescent development, the impact of violence and bullying on adolescent health and mental wellbeing, and brings together psychological, epidemiological, behavioural genetic and historical approaches to consider pathways to resilience across the life course.
Brain diaries.
Researchers from across the University, including experts focusing on infant neuroscience, contributed to an exhibition on the physical developments of the brain at Oxford University Museum of Natural History.
The ‘Brain Diaries’ exhibition was the product of a collaboration between more than 150 research scientists and over 20 support staff from four University departments, and explored how the brain develops from the fetal formation of the brain through to changes due to old age.
A playlist of videos from the 'Brain Diaries' exhibition at Oxford University Museum of Natural History
In response to the Brain Diaries exhibition, the Joint Museums Community Engagement team collaborated with the Headway Oxfordshire charity and poet Kelly Swain to create ‘My Brain Diaries’.
Participants in the project at the Headway Centre in Kennington near Oxford were given an introduction to the exhibition and a presentation on MRI Scanning by Professor Stuart Clare. Over 4 weeks, the group members then created visual poems, reflecting their own personal Brain Diary.
The impact of COVID-19 on child and adolescent mental health.

Wellbeing and resilience.
Mental health concerns often emerge during adolescence. Oxford researchers are investigating the ongoing mental health impacts of the COVID-19 pandemic on adolescents and their parents, including how lockdown measures, social isolation, physical distancing and uncertainty about the future resulted in high levels of anxiety and worry.
The ESRC-funded Oxford ARC study (Oxford Achieving Resilience during COVID-19) was launched to track adolescents’ mental health during the COVID-19 crisis – and to find out what promotes or hinders their mental wellbeing and resilience.
The researchers, including Professor Elaine Fox, now at the University of Adelaide, surveyed over 850 teenagers (aged 13–18) and their parents in the study, consulting with the TRIUMPH Mental Health Network’s Youth Advisory Group to better understand the impact of COVID-19 on common mental health issues relating to worry, anxiety, depression and eating-related problems.
Findings from the Oxford ARC study show that teenagers surveyed were twice as likely as their parents to feel lonely and isolated during the pandemic, despite spending time online.
Participants consistently reported that they feel unable to control the important things in life, with rates as high as 60%.
During lockdowns teenagers experienced higher levels of worry about missing school or work than their parents, and increasingly feel unable to cope with the unexpected.
‘... understanding how social isolation and the pandemic is affecting young people’s mental health is crucial.’
Experts at Oxford are looking not only at the mental health impacts of COVID-19, but also the solutions needed to address the issues that have arisen for young people.
A team of researchers, including Professor Cathy Creswell, provided policy guidance including 14 steps that schools, mental health services and policymakers can take to help children and young people whose mental health has been affected by the COVID-19 pandemic.
‘In seeking to limit the impacts of the pandemic on young people and provide much needed supports, we need a multi-pronged approach that incorporates actions in each of these settings.’
Lockdowns and mental health.
The COVID-19 pandemic significantly affected how teaching was delivered across all age ranges – but how did this impact the mental health of students in primary and secondary education?
Using data from the OxWell study, experts at Oxford investigated how lockdown had impacted the mental wellbeing of 17,000 UK school students (aged 8 to 18).
‘… for some children and young people we have seen reported benefits to their mental health and wellbeing during lockdown.’
They found that a third (33%) of students reported improved mental wellbeing during the first UK lockdown. By analysing the results from the self-reported survey, it was shown that students who reported better wellbeing during lockdown were also more likely to report positive lockdown experiences of school, home, relationships and lifestyle.
Compared to their peers, this group were also more likely to report decreases in bullying, improved relationships with family and friends, better sleep, and more exercise than before lockdown.
A further 32.9% of the respondents to the survey reported no change in wellbeing, whereas 33.9% reported a deterioration in wellbeing.
The study gives an insight into how individual and environmental factors may support children and young people to thrive throughout school disruption and adversity. Professor Mina Fazel, Chair of Child and Adolescent Psychiatry in the University’s Department of Psychiatry, says that further exploration, examination and reflection upon the experience of children and young people in the pandemic is ‘paramount to understanding how the reported benefits can be maintained for the millions of children and young people in education now and beyond the pandemic’.
The research survey Co-SPACE (COVID-19 Supporting Parents, Adolescents, and Children in Epidemics) was launched to track children and young people’s mental health throughout the COVID-19 crisis and identify ways to protect their mental health.
Oxford researchers Professor Cathy Creswell, and Associate Professor Polly Waite from the Departments of Psychiatry and Experimental Psychology, and Dr Simona Skripkauskaite from the Department of Experimental Psychology, were among the principal investigators of Co-SPACE.
A recent Co-SPACE report highlighted how younger children’s mental health had suffered as a result of lockdowns. Parents and carers reported behavioural, emotional and attention difficulties in their children during national lockdowns, and this was especially the case in primary school children.
More secondary school aged girls (11–17 years) were also reported to have experienced emotional problems than in previous months including feeling unhappy, worried, and experiencing physical symptoms associated with worry.
‘We are really concerned that in our study population we have once again seen increases in mental health symptoms across emotional and behavioural domains in primary school children in January – and also that emotional symptoms among secondary school girls are at the highest point that we have seen since we started our study in March 2020’
The researchers used findings from the study to contribute to the UK government’s State of the Nation 2021 report, looking at children and young people’s wellbeing.
‘Our findings demonstrate the extent of the impact of COVID-19 on children and young people's lives, especially for particular families’
Building on research from the Co-SPACE study, Dr Simona Skripkauskaite leads one of ten collaborative research projects jointly awarded by the Economic and Social Research Council (ESRC), the Arts and Humanities Research Council (AHRC) and the Japan Society for the Promotion of Science (JSPS), to address the challenges presented by the global pandemic.
Anxiety, depression and eating disorders.

Anxiety.
Anxiety disorders are the most common mental health disorders among children. Oxford researchers are working to assess child anxiety disorders and develop better treatment and diagnostic measures.
The Oxford Psychological Interventions for Children and adolescents (TOPIC) Research Group from the Department of Experimental Psychology undertook a qualitative study with the aim of informing clinical guidance on using child anxiety disorder diagnoses.
The team, including Dr Tessa Reardon, conducted in-depth interviews with 11 parents of children (aged 7–12) who had received an anxiety disorder diagnosis in order to find out more about their experiences of the diagnostic process.
They found that the process of receiving an anxiety disorder diagnosis can be a very helpful and positive experience for families, as it allowed parents to access professional support for their child, and helped them to feel more in control of the situation.
Parents also expressed some concerns about their child’s future and the negative consequences associated with the diagnostic ‘label’. For example, some parents were worried that their child would continue to experience anxiety problems into adulthood, or were concerned that other people would treat their child differently as a result of their diagnosis.
‘Our findings show how assessing and sharing anxiety diagnoses with families can be helpful and importantly highlight ways clinicians can help ensure it is a positive experience for families.’
Almost two-thirds of parents of children with an anxiety disorder report seeking help from a professional to help manage and overcome their anxiety difficulties.
Professor Cathy Creswell was awarded a £2.5 million grant from the National Institute for Health and Care Research to develop and evaluate procedures for identifying and treating anxiety disorders in primary school aged children in schools across the UK, as part of a wider multidisciplinary five-year research programme made up of researchers from around the University of Oxford: Online Support and Intervention for Child Anxiety (OSI).
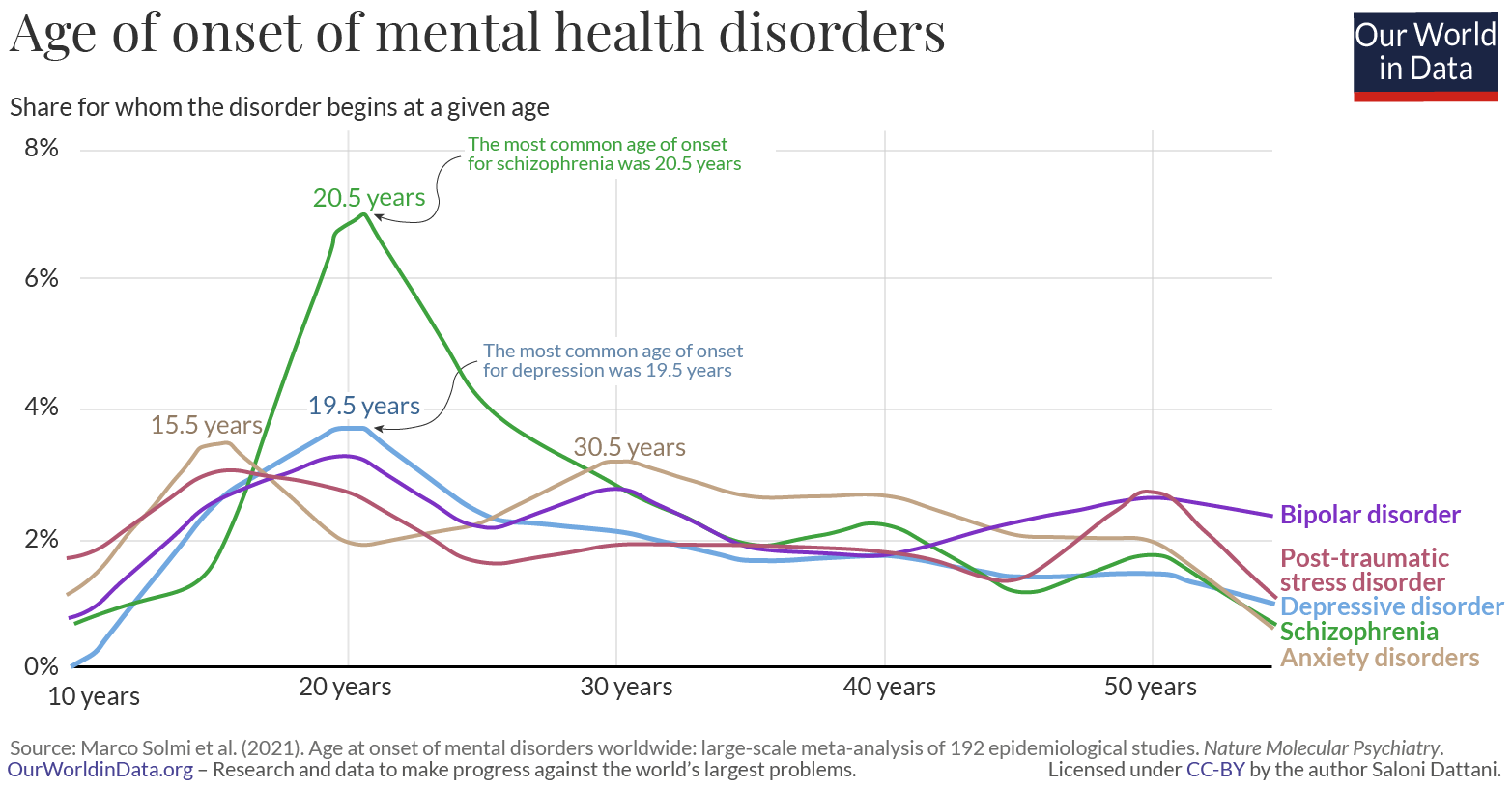
‘Anxiety disorders are the most common mental health problem across the life course, and often have their onset in the primary school years.’
Half of all lifetime cases of anxiety disorders begin before the age of eleven. Children who suffer from anxiety disorders are more likely than their peers to experience ongoing anxiety problems throughout life, develop other serious mental health disorders, and have reduced educational and employment opportunities.
The Minimising Young Children’s Anxiety through Schools (MY-CATS) trial is investigating whether an online programme delivered by parents and carers could be one approach to help increase access to mental health support. The programme, called OSI (Online Support and Intervention for child anxiety), is being tested on children ages 4–7 who are identified as at risk for anxiety problems through screening in primary schools.
Associate Professor Mara Violato from the Health Economics Research Centre at Oxford Population Health, will also lead a cost-effectiveness analysis of the OSI intervention. This will include both individual and broader societal measures, including health-related quality of life for both children and parents, use of mental health services, time off school for children, productivity losses for parents, and the costs to run the OSI programme.
‘We hope that MY-CATS will not only advance knowledge about risks for child anxiety disorders and their underlying mechanisms, but also influence health policy and practice by informing prevention and early intervention programmes.’
Researchers at from the Health Economics Research Centre are leading cost-effectiveness analyses for two trials aimed at improving screening and treatment for children with anxiety disorder.
The Child Anxiety Treatment in the context of COVID-19 (Co-CAT) trial will compare the clinical and cost-effectiveness of an online parent-led treatment for child anxiety problems with usual care delivered in Child and Adolescent Mental Health Services (CAMHS) in the UK throughout the COVID-19 pandemic to date.
The Identifying Child Anxiety Through Schools – identification to intervention (iCATS-i2i) trial will establish if systematic screening for anxiety problems in children, sharing screening outcomes with families, and the delivery of a brief parent-led online intervention through schools is both effective and cost-effective.
‘Identifying interventions for child anxiety problems that are both clinically effective and good value for money is of paramount importance.’
Treatments for anxiety.
Oxford’s experts are working to uncover the most effective treatments for young people with anxiety disorders.
Professor Andrea Cipriani from Oxford’s Department of Psychiatry authored a study examining group cognitive behavioural therapy (CBT) as a treatment for children and adolescents experiencing anxiety disorders.
Cognitive behavioural therapy (CBT):
Cognitive behavioural therapy (CBT) is a talking therapy designed to help people manage problems by encouraging positive behaviours in the way they think and behave
The study revealed that group CBT was significantly more effective in reducing anxiety symptoms than other psychotherapies and all control conditions immediately after treatment and at short term follow up.
‘This study is encouraging because it shows that there is real benefit in long-established psychological treatments for anxiety disorders in adolescents.’
Associate Professor Mara Violato and Professor Cathy Creswell contributed to a study comparing the clinical outcomes and cost-effectiveness of brief guided parent-delivered CBT and solution-focused brief therapy (a form of counselling that focuses on the present and future and explores a child’s resources and hopes to help build solutions).
Along with colleagues of the University of Reading, the team found no evidence of CBT being clinically superior to brief solution-focused therapy, but it was shown to be cost-effective in the short-term.
At the end of treatment 40 children (59%) in the brief guided parent-delivered CBT group had improved compared to 47 children (69%) in the solution-focused brief therapy group.
Depression.
Oxford’s experts are studying how adolescent depression increases the risk of violence.
The study, 'Depression and violence in adolescence and young adults: findings from three longitudinal cohorts', examined the association between depression and subsequent violence from three representative samples in the Netherlands, UK and Finland.
The research team was led by Professor Seena Fazel and senior researcher Rongqin Yu, from the Department of Psychiatry’s Forensic Psychiatry Group, and used data from the three cohorts to examine the links between adolescent depressive symptoms and violent behaviours from age 13 to 17.
The study found modest increases in risk of violence in depression, with one sample showing 7.1% of individuals with depression were convicted of one or more violent crimes, compared with 3.6% in the general population without depression.
The research revealed a consistent pattern of increased relative risk of later violence, highlighting the need for active and early treatment of depression in adolescents and young people.
‘... closer liaison between criminal justice and mental health might prevent violence in high-risk individuals.’
One of a series of Wellcome Trust reviews of the active ingredients of interventions to prevent and treat depression and anxiety in young people was carried out by the team in the Psychopharmacology and Emotion Research Laboratory (PERL) at the Department of Psychiatry.
‘It is important to understand the effects antidepressants have in young people so that they can make informed choices about the best treatment approach for them.’
Researchers, including Professor Catherine Harmer and Associate Professor Susannah Murphy, reviewed literature about the use of antidepressants in young people aged 14–24 years, and held a series of online workshops with young people with lived experience, which were supported by the McPin Foundation and the NEUROSEC (Neuroscience, Ethics and Society) Young People Advisory Group.
Professor Catherine Harmer and Dr Susannah Murphy featured on the National Elf Service podcast discussing the Wellcome Trust Active Ingredients project on antidepressants for young people with depression and anxiety.
Eating disorders.
Over 1.6 million people in the UK are affected by eating disorders, and the majority are aged 12–20. Eating disorders are complex mental health problems and deal with emotions, characterised by negative thoughts, perfectionism, obsessiveness, cycles of control and self-punishment as well as low self-esteem, depression and often self-harm.
Research led by the University of Oxford shows that people who suffer from recurrent abdominal pain in childhood may be more likely to have disordered eating as teenagers, and is the first study to provide prospective evidence of an association between recurrent abdominal pain at ages 7–9 years and fasting to control weight at age 16 years.
Oxford researchers, led by Dr Kate Stein from the Department of Psychiatry, with colleagues from Duke University and the University of Bristol, used the ‘Children of the 90s’ population cohort of 14,000 children in the UK to explore this association.
‘By enquiring about a history of childhood recurrent abdominal pain in all patients with eating disorders, we would be able to identify patients whose childhood pain may have contributed to their food avoidance and tailor their treatment plan accordingly’
Researchers from the Departments of Psychiatry and Experimental Psychology undertook a study examining links between anxiety, stress and binge eating tendencies in adolescence.
Researchers examined a group of adolescents aged 13 to 16 over three testing periods spaced 12 to 18 months apart, to investigate whether high levels of anxiety and stress interacted to increase likelihood of binge eating tendencies in individuals over time.
Results of the study revealed that participants who experienced higher anxiety and stress than usual were more likely to score highly on binge eating tendencies measures, compared to when they experienced lower levels of anxiety and stress.
The study recommends raising greater awareness in parents, educators, and health professionals of the link between high anxiety and stress and increased risk of binge eating tendencies, in order to facilitate better prevention, detection and early intervention.
Child and adolescent mental health in a digital world.

Wellbeing and digital treatments.
Previous research has shown that 75% of mental health problems emerge before the age of 24. Oxford researchers are doing crucial research to investigate how digital interventions can help prevent or reduce mental health problems.
The ATTUNE study is one of a number of projects being funded by a major £24 million investment from UKRI into improving the mental health and wellbeing of adolescents in the UK.
Led by Professor Kamaldeep Bhui in the Department of Psychiatry, it brought together diverse creative-arts, digital and health experts to investigate how adverse childhood experiences can affect adolescents' mental health.
‘...we aspire to transform social, education, health and care systems to provide therapeutic spaces and life opportunities for young people to flourish’
In a study conducted on behalf of ATTUNE, Professor Bhui and collaborators from Queen Mary University of London, Falmouth University and Imperial College London examined how digital and creative arts interventions can aid prevention and recovery from mental health consequences of adverse childhood experiences.
The study found promising results, especially when young people are engaged in the implementation of digital health interventions.
Professor Cathy Creswell is a co-applicant on another of the projects to receive UKRI funding.
The four-year research programme – Adolescent Mental Health and Development in the Digital World – will address the major societal challenge of building a safe and supportive online environment with the aim of preventing or reducing the emergence of depression, anxiety and self-harm in young people.
‘I am delighted to be involved in this exciting programme of work which aims to capitalise on the potential of digital technology to improve mental health among adolescents’
Researchers Professor Ilina Singh, from the Department of Psychiatry, and Dr Gabriela Pavarini, from the Department of Social Policy and Intervention, were awarded a British Academy Youth Futures grant for a research project aiming to advance understanding of youth agency in mental health and contribute to the achievement of a sustainable and healthy future for Brazilian youth.
Along with Professor Sheila Murta, University of Brasilia, the team work in collaboration with groups of adolescents in Brazil, to investigate their sense of agency toward mental health promotion, and develop a digital tool to do so.
‘Our systematic and co-productive research in Brazil should help us learn lessons in how young people and digital innovations can contribute to sustainable mental health and wellbeing across diverse contexts’
A group of researchers, including Dr Holly Bear from the Department of Psychiatry, investigated what proportion of smartphone apps are improving current issues facing services for young people’s mental health by improving the scalability of evidence-based mental health interventions.
They found that factors including high cost, funding constraints, and lengthy research processes impeded implementation.
Life online.
Young people are living their lives in fundamentally different ways from previous generations, with up to 96% of young people aged 16–24 engaged in social networking online.
Oxford’s experts have long been investigating the opportunities and challenges of the internet on young people’s mental health. Professor John Powell from the Nuffield Department of Primary Care Health Sciences conducted a study in 2011 exploring the mental health implications of internet use, and how practitioners could harness its benefits to minimise harm.
Researchers at the Department of Computer Science are exploring the impact of digital technologies on children’s health, wellbeing and autonomy.
Dr Jun Zhao leads the Oxford Child-Centred Design Lab, an initiative that brings together interdisciplinary researchers, industrial practitioners and policymakers together to explore new and ethical ways of building technologies for children.
In 2024, the team received a UKRI award to support the CHAILD (Children’s Agency in the Age of AI: Leveraging Interdisciplinarity) project, which investigates how children understand and experience algorithmic systems.
They also received an Impact Acceleration Award and an Innovate UK award to collaborate with the Lego Foundation in developing ethical design principles for children-focused innovation.
Her team works closely with families, schools and technologists to support children’s rights, agency and understanding in the digital world. This work builds on earlier projects including KOALA (Kids Online Anonymity & Lifelong Autonomy), co-led by Professor Sir Nigel Shadbolt and Dr Jun Zhao.
‘With technology now such an integral part of our daily lives and increasingly so for adolescents, it’s crucial we understand what’s driving these shifts in wellbeing and whether technology is a consistent underlying factor across all nations’
In a study from the Adolescent Well-Being in the Digital Age Programme researchers examined data from over 430,000 adolescents in the UK and US to investigate how associations between adolescents’ technology use and mental health have changed over the past 30 years.
Dr Matti Vuorre, a former member of Professor Przybylski’s team, found little evidence for increases in associations between adolescents’ technology engagement and mental health.
‘If we want to understand the relationship between tech and wellbeing today, we need to first go back and look at historic data - as far back as when parents were concerned too much TV would give their kids square eyes’
In a separate study, the first of its kind, researchers from the Oxford Internet Institute’s Adolescent Well-Being in the Digital Age Programme collaborated with experts from across the University of Oxford and found that engaging with arts and culture online can improve mental health in young people.
Led by Dr Rebecca J Syed Sheriff, from the Department of Psychiatry, the study was conducted in partnership with Oxford’s Ashmolean Museum and was co-authored by Helen Adams from Oxford’s Gardens, Libraries & Museums, and Professor Przybylski.
‘As far as we’re aware this is the first experimental study of online cultural experiences for mental health in young people’
The Oxford researchers conducted an online trial in which participants aged 16–24 were offered access to an online cultural experience, and then compared the impact on measures relating to depression and anxiety amongst participants.
The study found a link between engaging in online arts and culture and mental health, with over 24% fewer people reported clinically significant distress between the start of the pilot study.
In 2023, the ORIGIN project launched, where young people will help create an 'online museum' as a way of improving their mental health.
‘There is a rapidly emerging field of research into how participation in arts and culture can contribute to better health and wellbeing’
Researchers from the University of Oxford have also been investigating the impacts of digital gaming on young people’s mental health.
A recent study found that although many school-age adolescents spend considerable time gaming, it does not have a negative impact on their wellbeing.
The study, led by Dr Simona Skripkauskaite from the Department of Experimental Psychology, and Professor Mina Fazel from the Department of Psychiatry, examined data from the the OxWell Student Survey, one of the largest school surveys of adolescent health and wellbeing in England.
The researchers found almost one-third of students that answered questions on their gaming reported spending at least 3.5 hours each day playing games on any electronic device, and that most of the ‘heavy’ gamers were experiencing no negative effects with regards to their wellbeing and 44% of ‘heavy’ gamers reported higher wellbeing than those who play games less or do not play them at all.
‘... rather than worrying about the time spent playing video games, we should explore the opportunity of video gaming as a potential tool to find more affordable, creative and less stigmatising ways to reach and help adolescents experiencing emotional and behavioural difficulties’
A collaborative group of researchers from the Departments of Psychiatry and Experimental Psychology, with colleagues from the University of Reading, conducted a systematic review to evaluate how immersive virtual reality and digital gaming can be applied as interventions for the treatment of mental health problems in children and young people.
They found that, despite digital interventions being in very early stages, there is cause for optimism for their potential in treating mental health conditions, particular depression.
Child and adolescent mental health care and the mental health of care-experienced young people.

Working with young people on mental health care.
An international group of researchers, including experts from the University of Oxford, are working together to help better understand how young people can manage their own mental health.
‘This study will be addressing a key question in the development of big data resources for mental health: how to make these platforms acceptable to young people’
Funded by the mental health area team at Wellcome, and led by Sage Bionetworks, the project aims to help enable the identification of the next generation of treatments and approaches to prevent, intervene, manage and stop relapse of anxiety and depression in young people.
Using data from mobile phones and other connected technologies, the study will analyse the lived experiences of the participants’ mental health self-management. The researchers hope that this will provide insight into how young people’s daily activities and surroundings affect their health and how successful their health-management strategies are.
Analysing self-help management is important, as young people have reported a preference for relying on themselves when facing difficulties.
A report co-authored by Dr Tessa Reardon, Professor Cathy Creswell and Associate Professor Polly Waite from the Departments of Experimental Psychology and Psychiatry investigated why children and adolescents don’t seek and access professional help for their mental health problems.
96%
of survey respondents reported barriers to accessing mental health care such as limited mental health knowledge and perceptions of help-seeking
By conducting a systematic review of all studies where children and adolescents were asked about the barriers and facilitators to help-seeking and accessing professional support, the researchers found that the main reasons given by young people related to mental health stigma and embarrassment, a lack of mental health knowledge, and negative perceptions of help-seeking.
They highlighted the essential nature of the relationship between schools and mental health services, which enable young people and their families to access support that can minimise the logistical barriers.
They also suggested that mental health professionals should offer young people different ways to access help on their own – including digital tools.
Researchers, including Dr Melina Dristaki and Sungwook Kim, have also investigated how the use of digital communication between young people and their NHS clinicians changes the young person's engagement with their health care - and how to identify costs and necessary safeguards.
Young people aged 16-24 and clinicians in the NHS are using digital communication, such as mobile phone calls, texts, emails and internet-based phone calls (Voice over Internet Protocol (VOIP)), to improve engagement, though there are gaps in evidence as to how this might work, its cost, and ethical and safety issues.
The study, led by experts from the University of Warwick and King’s College London, found that using digital communication enables timely access for young people to the right clinician at the time it makes a difference to how they manage their health condition.
It can also enhance patient autonomy, empowerment, and activation. While challenging the nature of the boundaries of therapeutic relationships, it can also improve trust.
Researchers identified staff time as the main cost driver, though the offsetting of costs is likely elsewhere in the health service.
Other risks could include an increased dependence on clinicians, accidental disclosure of confidential information, and failures in communication.
The findings of the study suggest that, as NHS policy prompts more widespread use of digital communication, benefit is most likely, and harms are mitigated, when digital communication is used between patients and clinical teams they already trust.
The study also highlighted how clinical teams will require a proactive approach to ethics, governance and public safety.
Spending on child and adolescent mental health services.
Though digital health technologies are becoming used more widely across the NHS, there is a lack of evidence relating to the economic impact of digital consulting in the UK.
Researchers, again including Sungwook Kim and Dr Meline Dristaki, aimed to estimate the direct costs, and comparative benefits, associated with digital consulting at eighteen clinics serving young people aged 16-24 with long-term conditions.
Health professionals identified four potential economic impacts for the NHS – decreasing adverse events, improving patient wellbeing, decreasing waiting lists, and staff workload.
Nurses and physiotherapists were the greatest users of digital consulting, with teams appearing to use an efficient triage system. Staff did report concerns regarding the time spent digitally consulting, and there are still considerable gaps in evidence related to the cost-effectiveness of digital consulting.
This study did however identify important cost-related outcomes for assessment in future cost-effectiveness trials.
£100
spending £100 more on physical health services was associated with 9% lower spend in child and young person mental health per person aged 0-18
It is estimated that less than a quarter of young people with a mental health condition receive any help from specialist services – with this treatment gap reflecting a disparity between the needs and resources committed to the mental health of young people.
In England, the funding decisions relating to most child and adolescent mental health services (CAMHS) is taken by NHS Clinical Commissioning Groups (CCGs).
Spending levels are not predetermined, and CCGs are assigned an overall budget based on both the physical and mental needs of the local population.
It’s up to the CCGs to decide their spending priorities, however, there is a stark variation in spend on CAMHS by different CCGs, leading to a ‘postcode lottery’ in access to services.
Researchers from the Health Economics Research Centre and the Department of Psychiatry have investigated whether the rate of spend on child and adolescent mental health is influenced by competing demand for other services.
The study, co-authored by Professor Mina Fazel, Apostolos Tsiachristas and Stephen Rocks (now at The Health Foundation), highlights the extent of the trade-off between physical health spend and spend on child and young person mental health (CYP MH).
The researchers recognise the challenge that healthcare commissioners in England face when balancing competing needs but raised concerns around trade-offs.
They noted that the average spend on CYP MH per person aged 0-18 was £46, though there was considerable variation across Clinical Commissioning Groups from £2 to £127.
Whilst acknowledging that physical and mental health services can’t directly be treated as substitutes – as good physical health can support mental health and vice versa – they did observe that a spending £100 more on physical health services was associated with a 9% lower spend in CYP MH per person aged 0-18.
Child and adolescent mental health services (CAMHS).
Primary care practitioners are the main point of referral for specialist mental health services in many high-income countries.
In order to streamline referrals and introduce self and parent/carer referrals, Child and Adolescent Mental Health Services (CAMHS) are increasingly adopting a Single Point of Access (SPA).
Single Point of Access (SPA):
Single Point of Access (SPA) provides healthcare professionals with an alternative referral route for patients needing community health services
The adoption of a SPA in CAMHS involves a significant shift of responsibility from primary care towards CAMHS, who adopt a more active role as a gatekeeper for their service.
Experts from the Departments of Primary Care Health Sciences and Psychiatry, and the Health Economics Research Centre within Oxford Population Health, have been evaluating the adoption of a SPA as part of the Child and Adolescent Mental Health Service transformations in Buckinghamshire and Oxfordshire.
The researchers found that the introduction of a SPA has potential to improve young people’s access to mental health services and help more individuals and families access timely support.
They did, however, note that the SPA does not in itself expand the Child and Adolescent Mental Health Service capacity – therefore expectations need to be tempered accordingly.
The same group of researchers, including Professor Mina Fazel, Apostolos Tsiachristas, Dr Margaret Głogowska, Stephen Rocks and Dr Melissa Stepney, later assessed how reorganisation in CAMHS affects access to services.
Antidepressant prescriptions.
Experts from the universities of Nottingham, Southampton and Oxford analysed trends in antidepressant prescriptions in children and young people in England for a period of approximately 20 years.
Using data from 1998 to 2017, the researchers, including Professor Andrea Cipriani from the Department of Psychiatry and Professor Julia Hippisley-Cox from the Department of Primary Care Health Sciences, aimed to describe trends and variations in prescriptions that have been increasing in number for children and young people.
37%
of children and young people prescribed antidepressants in English primary care had a record of visiting an NHS-funded paediatric or psychiatric specialist less than 12 months before or 6 months after their first antidepressant prescription
Analysing secondary care specialist visits made by children and young people prescribed antidepressants in secondary care, the researchers suggest that many children and young people are being prescribed antidepressants without the recommended involvement of a relevant specialist.
They suggest that their findings may justify greater training for GPs and great access to specialist care and non-pharmalogical treatments.
Paranoia and mistrust in adolescents attending mental health care.
Little research has been conducted into excessive mistrust in young people, despite paranoia being a potentially significant concern during adolescence.
Dr Jessica Bird, Professor Daniel Freeman and Dr Felicity Waite worked with colleagues from Child and Adolescent Mental Health Services (CAMHS) within Oxford Health NHS Foundation Trust to conduct the first longitudinal study to examine the predictors of paranoia persistence in adolescents with mental health problems.
The study set out to test cognitive, affective, and social factors in the early development of paranoia.
Paranoia:
A medical condition or symptom of a medical condition characterised by delusions
Working with adolescents aged 11-16, the researchers found that significant predictors of paranoia persistence included anxiety, depression, worry, negative self-beliefs, perceptual anomalies (such as hallucinations), insomnia, bullying and cyber-victimisation.
As excessive mistrust may be corrosive for adolescent social relationships – especially in the context of mental health disorders – the researchers then conducted a larger study to examine prevalence, symptom associations, and persistence of paranoia in a cohort of young people attending CAMHS.
54%
of participants in the study thought that people were lying to them on purpose
The researchers found that, as expected, the adolescents attending CAMHS were primarily doing so for reasons such as anxiety and depression, however, rates of paranoia in the cohort were approximately double those observed in adolescents from the general population.
Following this, the researchers conducted a study looking further into the journey of adolescent paranoia.
They interviewed twelve adolescents aged 11-17, starting with their awareness of paranoia, the beginnings of their paranoid experience, and their adjustment to paranoia in daily life.
They found that paranoia in adolescence involves navigating multiple tensions – as young people balance their independence with vulnerability, trust with mistrust, and the desire to be social with a fear of danger and deception.
All interviewees had paranoid worries of physical harm from others, although social, emotional and sexual harms were also described.
One of the insights from the study highlighted that, though sexual harm is a threat to all, girls especially may feel vulnerable in adolescence as they discover the realities of sexual harm.
The participants in the study described how this is further emphasises to girls through the media, warnings from adults, and their friends – with a 2018 Girlguiding survey showing that 30% of adolescent girls knowing other girls their age who have been sexually assaulted.
‘Our research highlights the importance in understanding how childhood sexual abuse leads to conditions such as substance misuse or psychiatric conditions’
Researchers from the Department of Psychiatry have also investigated the link between sexual abuse and mental health conditions, suggesting that earlier mental health support for victims would reduce the chances of victims developing psychiatric conditions, and substance misuse, in later life.
The mental health of care-experienced young people.
Adolescents are the fasting growing age group entering care in England, and adolescents entering care are six times more likely than the general population to experience mental ill-health. Despite this, evidence indicates that the mental health needs of adolescents with social-care experience are under-reported and under-treated.
1 in 30
UK children are taken into care at some point before their 18th birthday, with many experiencing abuse, neglect and other difficulties
Collaborating with colleagues from the University of East Anglia and University College London, Claire Duddy and Dr Geoff Wong from the Nuffield Department of Primary Care Health Sciences, are aiming to assess whether an intervention called Life Story Work (LSW) can improve the mental health and mental health support available to adolescents with social-care experience.
‘Our research highlights the importance in understanding how childhood sexual abuse leads to conditions such as substance misuse or psychiatric conditions’
A research programme investing factors linked to the mental health and wellbeing of care-experienced young people moving from primary to secondary school, and moving from adolescence to adulthood, received £2.8 million in funding.
Led by an interdisciplinary team from the Universities of Oxford and Bath, in collaboration with colleagues at Cardiff University, the programme aims to identify key processes linked to the mental health and wellbeing of care-experienced young people – particularly focusing on psychological processes and the role of support systems and services to identify targets for future intervention and prevention programmes.
Protecting child and adolescent mental health in crisis contexts.

Helping parents support childhood mental health in a crisis.
Researchers from Oxford’s Department of Social Policy and Intervention are producing resources for parents to support the mental health of children in crisis contexts.
Developed and tested by Dr Jamie Lachman, Professor Lucie Cluver, and Professor Frances Gardner, the award-winning Parenting for Lifelong Health (PLH) initiative was created in collaboration with the World Health Organisation (WHO), UNICEF, the United Nations High Commissioner for Refugees (UNHCR) and the United Nations Office on Drugs and Crime (UNODC), as well as academic colleagues from South Africa and the United Kingdom.
Find out more about how researchers are producing resources for parents to support the mental health of children in crisis contexts
Having reached over 15 million families in Ukraine and Pakistan, the Parenting for Lifelong Health team have worked with organisations including the WHO, UNICEF, UNHCR and UNODC to create rapidly shareable social media assets and resources following the devastating earthquakes in Turkey and Syria.
Based on 15 Oxford-University led randomised control trials of parenting interventions, the assets and resources include invaluable tips for parents and caregivers and are available in Turkish, Arabic and English.
More from PULSE.