Parental and maternal mental health.
From understanding fetal neurodevelopment in pregnancy to analysing the impacts of parental psychosis, researchers at the University of Oxford are changing the way we think about parental and maternal mental health.
They’re standardising global measurements for fetal brain growth and working with theatre directors to raise awareness of women’s lived experiences of mental illness during pregnancy and after birth.
Our experts are shaping global policy and – crucially – improving mental health outcomes for both parent and child.
Content warning:
Please be aware that this page refers to depression, anxiety, psychosis and topics such as maternal suicide.
Tags:


Understanding the early brain through fetal neuroscience.
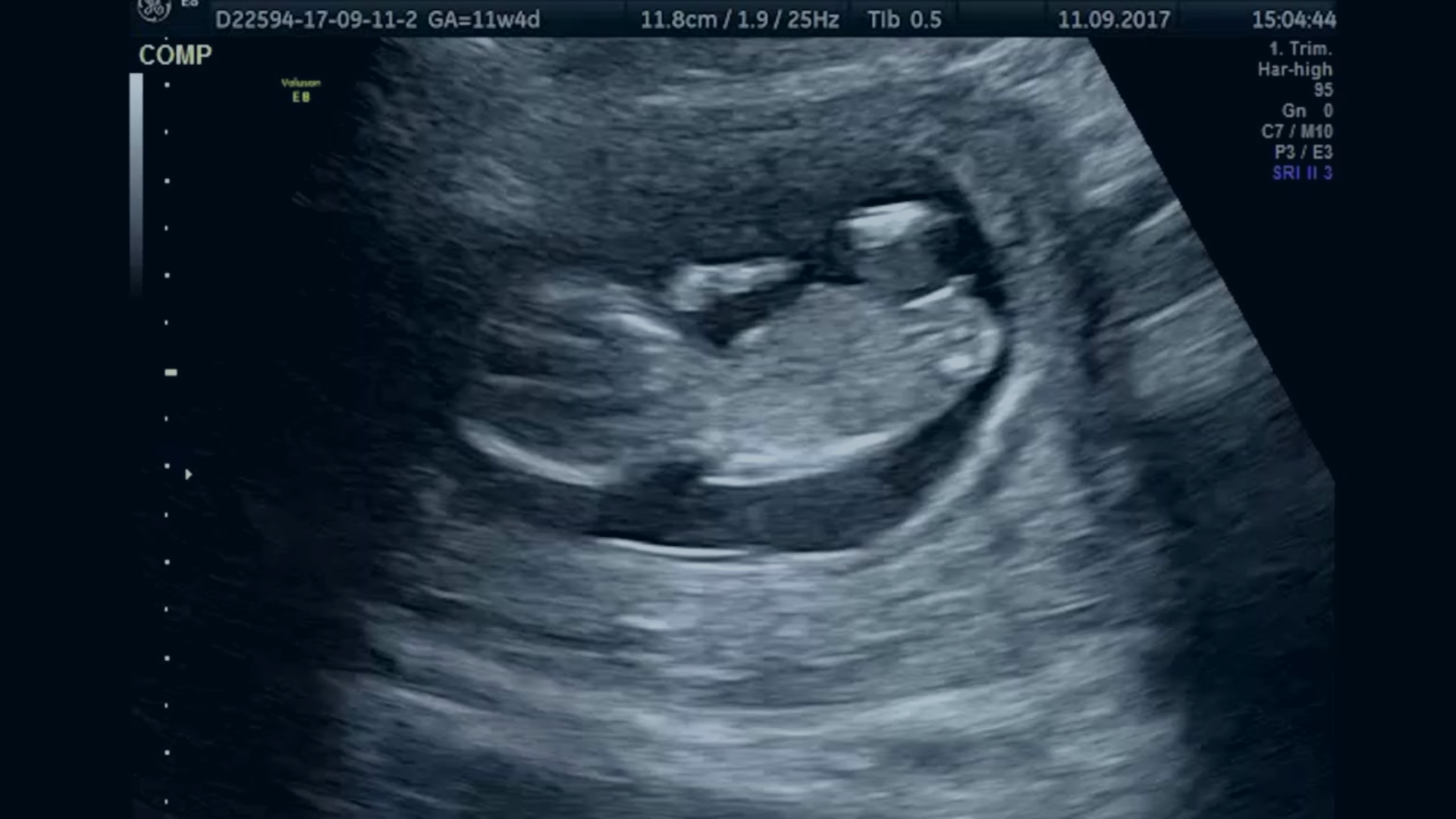
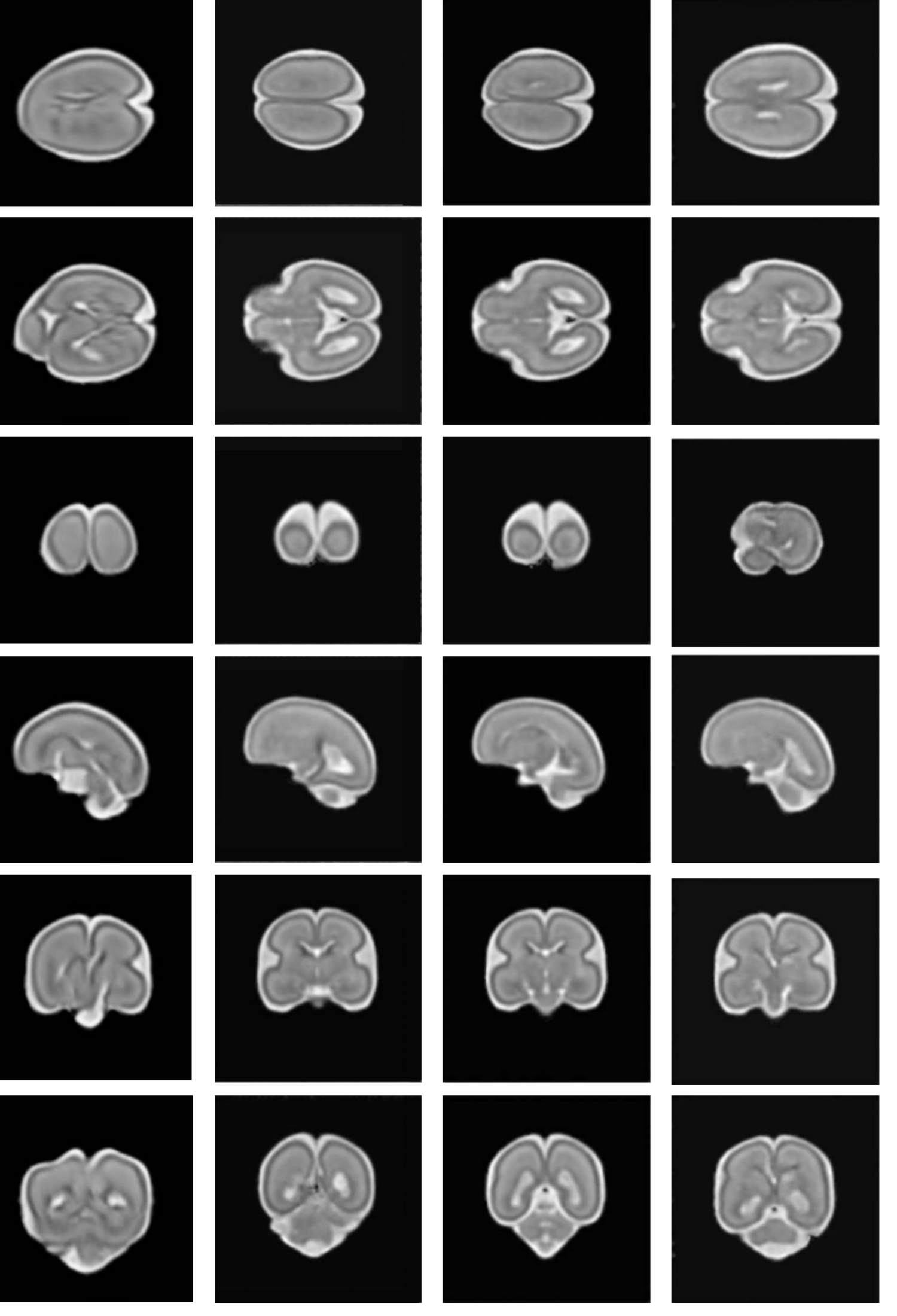
Fetal neuroimaging.
The fetal brain undergoes significant changes as a baby develops, so Oxford researchers are working to improve fetal ultrasound analysis and better standardise global measurements for fetal brain growth.
The Noble Group at the Institute of Biomedical Engineering looks at questions such as why ultrasound scanning and interpretation is so hard to learn, whether AI can simplify ultrasound and whether computers can mimic what a skilled sonographer can do.
A long-standing collaboration between colleagues from the Noble Group and the Oxford Maternal and Perinatal Health Institute (OMPHI), part of the Nuffield Department of Women’s and Reproductive Health, has led to a number of advancements in this area.
One such collaboration proposed an automated framework for predicting age and neurodevelopmental maturation of a fetus based on 3D ultrasound brain images. This is particularly important, as accurate estimation of gestational age is essential to prenatal care.
The team, which included Professor Ana Namburete (founder of the Oxford Machine Learning in Neuroimaging Lab), Professor Alison Noble and Professor Aris Papageorghiou, developed a new feature-based model that had never before been attempted. Their analysis showed that the model did not just estimate chronological age, but also the neurodevelopmental stage of the fetus based on brain structure.
Neuroimaging:
Any non-invasive means of generating images of a living brain. These are used for diagnosis of brain disease and injury and can also be obtained to show activity in the brain as various mental tasks are being performed
A later collaboration between these colleagues, which also included Postdoctoral Researcher Jianbo Jiao, formerly of the Department of Engineering Science, looked at second-trimester anomaly screening in the fetal brain.
While fetal brain magnetic resonance imaging (MRI) offers detailed images of brain development, they are not used in the second trimester due to time and cost limitations. In this case, ultrasound (US) is then employed.
Expert sonographers are adept at reading ultrasound images, but MR images are easier for non-experts to interpret. By developing methods to synthesise MR-like fetal brain images from ultrasound ones, the researchers hope their framework can be useful when communicating ultrasound findings to both obstetricians and patients.
Working with Dr Lorenzo Venturini (DPhil 2022), Professors Namburete, Noble and Papageorghiou also co-authored a paper exploring the use of convolutional neural networks, or CNNs, for the segmentation of multiple fetal brain structures in 3D ultrasound images.
Convolutional neural network (CNN):
A convolutional neural network (CNN) is a machine-learning technique that can learn to distinguish important boundaries and objects; they are increasingly popular in the segmentation of fetal ultrasound images
The proof-of-concept paper looked at whether the researchers could apply a machine-learning based method for automated segmentation of multiple fetal brain structures. This sort of accurate detection can track brain development through gestation, helping predict fetal health outcomes.
Additional work on the topic of CNNs has been conducted in collaboration with the Big Data Institute, the Oxford University Centre for Integrative Neuroimaging and the INTERGROWTH-21st Consortium.
Titled BEAN (Brain Extraction and Alignment Network), the collaborative paper presents a multi-stage CNN that allows for the actual shape of the brain to be analysed, which is fundamental to tracking how the brain matures.
Setting standards for growth.
The INTERGROWTH-21st (International Fetal and Newborn Growth) Consortium, which is dedicated to improving perinatal health, also looked at creating standards for five fetal brain structures.
Fetal brain anatomy is assessed routinely as part of the 20-week anomaly scan. The measurements are assessed against one of several reference charts. However, these have limitations, and there can also be a lack of consistency in the interpretation of ultrasound images of the fetal central nervous system.
Using a study population consisting of women at low risk of adverse pregnancy and perinatal outcomes, the researchers produced international size standards for fetal brain ultrasound measurements.
Perinatal:
Technically, the perinatal period starts at the onset of labour, and lasts until the restoration of the maternal uterus and the adjoining region. For statistical purposes, this period last from the 28th week of pregnancy until the end of the first week of the infant’s life
Alongside developing standards for fetal brain structures, researchers in the INTERGROWTH-21st project, which involved nearly 60,000 mothers and babies in eight urban areas in Brazil, China, India, Italy, Kenya, Omen, the UK and the USA, were also able to develop international standards for fetal cerebellar growth and Sylvian fissure maturation.
Cerebellar:
Relating to the part of the brain at the back of the skull that coordinates and regulates muscular activity
Analysing fetal development.
In addition to setting standards for fetal growth, experts at Oxford are analysing some of the ways in which fetal development can be affected.
For example, a paper co-authored by Professor Aris Papageorghiou looked at the development of the fetal nervous system, and how this could be affected by Brain-Derived Neurotrophic Factor (BDNF) levels in second trimester amniotic fluid. This is important as abnormalities in fetal growth can be linked to maternal, fetal and neonatal adverse outcomes.
A paper co-authored by Professor Aris Papageorghiou, Professor Ana Namburete and colleagues from Leiden University also analysed fetal brain development to help understand whether changes in fetal circulation contributes to the delay in maturation of the cortex in fetuses with congenital heart defect (CHD).
Mental health in pregnancy.

Depression and anxiety in pregnancy.
Experts at Oxford are not only working to improve aspects of fetal neuroscience, but also to improve the mental health and wellbeing of expectant mothers during pregnancy.
A study co-authored by Professor Alan Stein revealed a generational increase in depression and anxiety in young pregnant women. The study demonstrated that young women are 51% more likely than their mothers to experience depression and anxiety during pregnancy.
Following women during their pregnancy in the 1990s, and their daughters as they become mothers, the study is thought to be the only one in the world to have identically tested women across two generations.
It found that a 25% of the women today who became pregnant before the age of 24 exhibited ‘high depressive symptoms’, compared to 17% of the original group.
Factors such as the rise in house prices and cost of living added to the levels of stress and anxiety, with researchers also highlighting the importance of the study’s findings for health services due to the impact of depression in pregnancy on both mother and child.
As part of the Mothers and babies: reducing risk through audits and confidential enquiries across the UK (MBRRACE-UK) collaboration, Oxford researchers are analysing the number of women dying as a consequence of complications during or after pregnancy.
Produced by the National Perinatal Epidemiology Unit, part of Oxford Population Health, MBRRACE-UK’s annual ‘Saving lives, improving mothers’ care’ report highlights maternal suicide as the leading cause of death during the first year after pregnancy.
Released in 2022, the report’s updated figures show that in 2020, women were three times more likely to die by suicide during or up to six weeks after the end of pregnancy compared to 2017-19. Deaths from mental health-related causes (including suicide and substance abuse) account for nearly 40% of deaths occurring within a year after the end of pregnancy.
The MBRRACE-UK collaboration also investigated persistent inequalities and continued inequitable care for pregnant women, highlighting the need for great coordination between care services – including GPs, maternal services and mental health services.
Professor Marian Knight explains the MBRRACE-UK report (2018)
Marian Knight, Professor of Maternal and Child Population Health and lead for the MBRRACE-UK collaboration, was appointed Member of the Order of the British Empire (MBE) for services to Maternal and Public Health in the New Year Honours list 2023.
Mental illness is estimated to affect one in ten pregnancies, and as the MBRRACE-UK figures show, has been found to be a leading cause of maternal mortality. Based in the National Perinatal Epidemiology Unit, the UK Obstetric Surveillance System (UKOSS) has been investigating antenatal suicide attempts – an area where no national data for ‘near miss’ suicide events exists.
Depression and suicide in pregnant migrants and refugees.
In addition to studying maternal depression and suicide in a UK-based cohort, Oxford experts are looking at how depression affects pregnant women in refugee and migrant populations.
Antepartum depression affects around 15% of pregnant women worldwide, and migrant women in resource-poor settings are disproportionately affected. Focusing their study on migrant women on the Thai-Myanmar border, researchers, including Professor Rose McGready and Dr Gracia Fellmeth, are exploring what refugee women who live along the border are perceiving as being contributory and protective factors to their antepartum depression.
Antepartum:
Occurring before the onset of labour
The study, with co-authors from the Shoklo Malaria Research Unit and the Universities of Leeds and Southampton, found that major themes such as financial problems, interpersonal violence and substance misuse among partners contributed towards persistent antepartum depression.
Factors such as social support, accessible healthcare and distractions were considered as being able to help protect mental wellbeing.
Postpartum and maternal mental health.

Analysing the impact of postpartum and maternal mental health issues.
Conducted by the National Perinatal Epidemiology Unit, the ‘You & your baby’ survey is one of several National Maternity Surveys that researchers have conducted using data going back almost two decades.
Forming part of the Policy Research Unit in Maternal and Neonatal Health and Care (PRC-MNHC), the surveys explore women’s health and experiences of care around the time of pregnancy, providing a snapshot of care and points of comparison over time. The survey results are then used to help improve maternity care throughout the country.
The survey results are then used to help improve maternity care throughout the country.
Results from the 2020 ‘You & your baby’ survey were gathered from a random sample of 16,000 women aged 16 and over who had given birth in October 2017. This was the first national maternity survey in England to ask women about their health and wellbeing six months after childbirth.
The results highlight the ongoing need to address maternal mental health problems and to offer women the support they need. 13% of women reported suffering from anxiety and 7% from depression during pregnancy, increasing to 29% of women reporting anxiety and 16% reporting depression during the postnatal period.
Research from the University and its partners is helping to influence national and global policy on maternal health. Experts are working with organisations such as the WHO on the health care of pregnant refugee and migrant women and new-born children, as well as the management of sepsis and maternal mental health.
Their findings are also highlighting inequalities in maternal health care, showing that black women are five times more likely to die than white mothers in pregnancy and childbirth.
‘We’re very proud that our policy and public engagement has helped change the conversation about maternal health inequalities and stigmatised conditions such as mental health.’
Experts from the Department of Social Policy and Intervention (DSPI) have also been recommending the commissioning of Specialist Health Visitors and in Perinatal and Infant Mental Health throughout the UK to help tackle the growing social cost issue.
These Specialist Health Visitors have an important role in supporting both health visitors and families at risk of, or already experiencing, mental health problems during the perinatal period.
Findings from the study conducted by the DSPI found that Specialist Health Visitors in Perinatal and Infant Mental Health constitute just 0.8% of the health visiting workforce. In some areas, funding for posts had never been allocated, and in others, the funding had been discontinued or cut.
Perinatal mental health issues can have a devastating impact on women and their families, but Specialist Health Visitors in Perinatal and Infant Mental Health can help. A survey of individuals in such roles found that they are focusing their casework on areas such as parental antenatal depression, antenatal anxiety, general anxiety, birth trauma, postnatal depression and panic attacks, using a range of interventions including listening visits and motivational interviewing.
From a purely financial point of view, perinatal mental health issues result in a cost of £8.1 billion for each one-year cohort of births in the UK. Respondents to the survey that formed the study highlighted a lack of funding in the area as the biggest barrier to promoting perinatal and infant mental health (PIMH).
Melita Walker, Head of Mental Health at the Institute of Health Visiting, welcomed the report, highlighting ‘how a well-resourced health visiting service, as part of the PIMH system, can maximise the opportunity for good family mental health and wellbeing.’
Global maternal mental health.
Led by Dr Gracia Fellmeth, the Perinatal Mental Health Study (PMHS) is a study of women’s mental health across two sites in India.
Part of the National Perinatal Epidemiology Unit, the study is looking to understand mental health problems that are common in pregnancy and after giving birth – for example depression, anxiety, PTSD or suicidal thoughts.
Associated with the Maternal and Perinatal Health Research Collaboration, India (MaathRI), the researchers conducting the study will first interview women in focus groups to ask about their knowledge of mental disorders such as depression and anxiety.
They will then test screening tools (questionnaires) that ask about symptoms of mental disorders, and finally, they will look to measure how common mental disorders are during pregnancy and after giving birth in these communities.
Also looking at improving women’s life-long health in India is the SMARThealth Pregnancy programme, led by Professor Jane Hirst from the Nuffield Department of Women’s and Reproductive Health, and Dr D Praveen from the George Institute for Global Health.
The programme aims to help community health workers at risk during pregnancy, hoping to improve pregnancy outcomes and prevent future health complications. The team are developing a low-cost tool to support the mental health of women during the first postnatal year in a study led by Senior Postdoctoral Researcher in Implementation Science Dr Nicole Votruba.
In addition to addressing maternal mental health concerns globally, Oxford experts are helping to investigate standards and structures of perinatal psychiatric training in Europe.
A paper co-authored by Dr Howard Ryland, Senior Clinical Researcher in the Department of Psychiatry, highlighted that, from a survey of 34 countries that are part of the European Federation of Psychiatric Trainees (EFPT), only six reported that specialist training in perinatal mental health was available.
Raising awareness of postnatal depression.
Researchers from the National Perinatal Epidemiology Unit (NPEU) are also developing innovative ways in which to raise awareness, reduce stigma and encourage discussion about maternal mental health.
A product of the collaboration between playwright Zena Forster, producer Emma Dolman, director Grace Duggan, and researchers from the NPEU, ‘after birth’ is a play that draws on the findings of original research and women’s lived experiences of mental illness during pregnancy and after birth.
Staged at the North Wall theatre in Oxford, the play was developed with women from the national charity Action on Postpartum Psychosis and part-funded by the University of Oxford’s TORCH Theatres Seed Fund.
The play was inspired by the research evidence and key health messages from the MBRRACE-UK investigations into maternal deaths, and uses humour to offer a life-affirming portrait of resilience and survival. In 2020 it was announced that ‘after birth’ had been named as the winner of the North Wall’s Propeller programme.
‘The play promotes some key public health messages about postnatal mental health, but importantly it’s also funny and full of hope.’
Parental mental health and its impact on children.

Familial influence on the mental health of children.
Maternal mental health is often associated with an increased risk of emotional and behavioural problems in children. However, the impact on children from the mental health of other family members has been given less attention.
A study co-authored by Professor Alan Stein, has taken a more generational approach by investigating the impact of grandmothers’ mental health on the emotional and behavioural development of their grandchild.
The results from the study showed that the associations between grandmothers’ and grandchildren’s mental health symptoms were comparable to maternal associations. There was no evidence for paternal associations, and there were stronger associations from maternal grandmothers compared to paternal ones.
From a purely paternal point of view, research co-authored by Professors Anne Goreily and Andrew Wilkie from the Radcliffe Department of Medicine, looked at the mechanisms behind why there is an increased risk of neurodevelopmental disorders such as schizophrenia and autism in the children of older fathers.
‘The risk calculator that we have developed is a tool meant to assist clinicians with identifying those young people who might benefit from closer monitoring and to motivate healthy lifestyle choices, and the reduction of modifiable risk factors, such as sleep regulation, substance use and exercise’
Family history is also a significant risk factor for bipolar disorders, though the magnitude of risk varies between individuals within and across families.
A study co-authored by Visiting Professor Anne Duffy, Dr Sarah Goodday and colleagues from multiple Swiss and Canadian universities assessed a risk calculator that could be used to predict a mood disorder in five to ten years for a young person with a confirmed first degree (ie parental) relative that has a bipolar disorder diagnosis.
The researchers found the tool to be correct approximately 70% of the time, with the study suggesting that it may be a useful clinical tool to help improve individualised risk estimation for adolescent offspring of a parent with bipolar disorder.
Bonding, criticism and parental attitudes.
A study published by the National Perinatal Epidemiology Unit explored how men’s attitudes towards fatherhood can affect children’s behaviour.
Researchers gathered information about parents’ mental health and socioeconomic status, and identified three areas of paternal involvement – a father’s emotional response to the child, the frequency of his involvement in housework and childcare activities, and his feelings of security in his role as a parent and as a partner.
Children whose fathers had a sense of security in their role as parent, and who were more positive about the role, were less likely to show behavioural difficulties by the time they reached ages nine and 11.
Father-child interactions in early infancy also positively influence children’s cognitive development, according to a study co-authored by Professor Alan Stein and Professor Paul Ramchandani, now LEGO Professor of Play in Education, Development and Learning at the University of Cambridge.
Parental behaviours and attitudes can, however, also have a negative impact on the mental health of their children.
For example, a study co-authored by Professor Cathy Creswell from the University’s Departments of Experimental Psychology and Psychiatry highlighted the correlation between parental criticism and adolescent internalising symptoms such as anxiety and depression.
A study co-authored by Myra J Cooper also investigated the connection between parental bonding and disrupted early parent-child relationships with eating disorder related conditions and negative self-belief.
Parental psychosis and psychological disorders.
Parental mental illness, including psychosis, is a well-established risk factor for children. Furthermore, children who experience parental psychosis are more likely to have their own behavioural and emotional difficulties during childhood.
With one in three people with a psychotic disorder also being a parent, experts at Oxford have been investigating the impacts of parental psychiatric disorders on the parent, and the wider family unit.
Professor Alan Stein reviewed research that links intergenerational transmission of parent psychiatric disorder and physical illness to psychological outcomes for children.
Alan and his co-author explore the different disorders that might affect parents, such as depression, anxiety and eating disorders, highlighting how more needs to be done to improve child outcomes and support families. They also raise the need for more research to be conducted in low- and middle-income settings.
Further exploration into how parental psychosis affects the wider family has been conducted by Dr Jessica Radley (now at King’s College London), alongside Professor Jane Barlow from the Department of Social Policy and Intervention, and Dr Louise Johns from the Department of Psychiatry.
One such study compares and contrasts family members’ perspectives of parental episodes of psychosis.
Conducting interviews with five families, the researchers explored how parental psychosis impacts the whole family, but how the role of being a parent can also be a source of hope.
The study found that the families involved often had poor mental health knowledge, and secrecy was common between parents and children, resulting in confusion and children being ill-informed about what their parent was experiencing.
The researchers identified a need for more work to be done to help reassure and motivate parents to communicate with their children about parental psychosis. They also highlighted how clinical settings could be improved to minimise the effects of separation by provision of an isolated, family friendly safe and comfortable environment for parents and children to be reunited after hospital stays.
The same group of researchers, Drs Radley and Johns, alongside Professor Barlow, also examined the experiences of mental health professionals who work with parents with psychosis and their families.
This study demonstrated a belief from the mental health professionals interviewed that the needs of parents with psychosis are contextual to their environment and level of psychosis symptoms, as well as other factors such as support from a partner sharing parental responsibilities.
The researchers highlighted the range of viewpoints that could exist within a team of mental health professionals and raised the need for ensuring that mental health professionals are given the necessary training in order to work with patients more holistically.
Parental anxiety and depression.
The impacts of parental anxiety and depression on children have been examined within the broader picture of parental psychosis; however, experts at Oxford have also delved further into how these two conditions in particular affect parental mental health and child mental health outcomes.
A study co-authored by Professor Cathy Creswell with colleagues from the University of Reading examined the association between parental responsibility beliefs, maternal anxiety and parenting behaviours in the context of childhood anxiety disorders.
The researchers developed a questionnaire for both anxious and non-anxious mothers of 7- to 12-year-old children with a current anxiety disorder. The results found that parents who also had a current anxiety disorder felt a great sense of responsibility for their child’s actions, while also highlighting that consideration of high parental anxiety and parental responsibility beliefs in the treatment of child anxiety may enhance outcomes.
Professor Creswell has also studied parental overprotection and how this might impact the development and maintenance of childhood anxiety disorders.
Researchers from the Nuffield Department of Primary Health Care Sciences, led by Dr Catia Nicodemo, are aiming to increase what is known about the negative effects of maternal depression and anxiety disorders on the mental health outcomes of children.
In a two-year study, they are hoping to estimate the indirect effects of maternal depression and anxiety disorders, and evaluate whether school and health policies might have a role in addressing the negative effects of the condition on children.
Parental depression and anxiety increase the risk of attachment, emotional and behavioural difficulties in children, with long-term implications for interpersonal relationship difficulties, educational and human capital outcomes. This is magnified in economically and socially disadvantaged communities in low-middle income countries, such as South Africa.
A study led Professor Alan Stein, based in rural South Africa, is developing guidelines for communicating to children about parental depression.
Factors such as the COVID-19 pandemic, and accompanied school closures, are significant psychological stressors for parents and families, exposing children to even higher levels of parental anxiety and depression.
The researchers in the study hope that by broadening their research to include communication with children about parental depression, anxiety and psychological distress, they develop evidence-based guidelines for healthcare workers to support parents on how to communicate effectively about their mental illness.
Parental mental health and COVID-19.
Led by Associate Professor Polly Waite and Professor Cathy Creswell from the Department of Experimental Psychology, the Co-SPACE study was set up to help us understand the impact of the COVID-19 on the mental health of families.
Conducted in collaboration with University College London, and funded by both the UK Research and Innovation Council (UKRI) and the Westminster Foundation, the study released an interim set of results in May 2020 – under two months after the start of the UK’s first lockdown.
From 5,000 responses to the study’s survey, the researchers found that work was the most frequent source of stress for parents, and that 80% of families who were previously receiving support from services said that they had been postponed or stopped.
Parents of children with Special Education Needs (SEN) and neurodevelopment disorders also reported higher levels of stress across all areas.
By June 2020, more than 10,000 parents had taken part in the Co-SPACE survey, which by then included questions around how parents felt about their children returning to school.
Half of the UK parents surveyed at that time did not feel comfortable about their children attending school following lockdown, with parents from lower income households being less comfortable than those with higher income.
Parents and carers highlighted their concerns about the practicalities of children returning to school, such as managing social distancing as well as their children, or them, catching or transmitting COVID-19.
‘Our data highlight the particular strains felt by parents during lockdown when many feel that they have been spread too thin by the demands of meeting their children’s needs during the pandemic, along with home-schooling and work commitments’
The November and December 2020 increase in COVID-19 restrictions, saw parental stress, depression, and anxiety again increase.
Researchers noted that this reflected symptoms such as difficulty relaxing, being easily upset or agitated, feeling hopeless, and lacking interest and pleasure, feeling fearful and worried, as well as being more irritable, over-reactive and impatient.
Commissioned by UK Department for Education on the recommendation of the Scientific Advisory Group for Emergencies (SAGE), the International Public Policy Observatory (IPPO)’s Rapid Evidence Review was released in September 2021.
Co-authored by Professor Creswell, the review synthesised research evidence from 32 studies on harms relating to the impact of lockdown and school closures on UK parents and carers.
It concluded that parents and carers had been disproportionately affected by school-closures, with research evidence showing increases in mental health problems, financial struggles, and an increased risk of violence within the home.
‘The COVID-19 pandemic has brought substantial challenges for parents and carers of children and young people. Our review has highlighted the negative impacts on parents and carers both economically and in terms of their mental health, particularly for families who already faced disadvantages.’
A paper published by Dr Simona Skripkauskaite, Samantha Pearcey, Professor Creswell and Dr Waite alongside colleagues from the Universities of Reading, Exeter and Southampton, examined how parental mental health symptoms changed throughout the course of the COVID-19 pandemic.
Using data from the Co-SPACE study, and partner Co-SPYCE study, the researchers found that parental stress and depression were higher during periods of restriction, but not anxiety – something that was most pronounced for parents with primary school-aged children.
The COVID-19 pandemic not only increased instances of parental stress and depression, but also increased pre-existing inequalities for mental disorders in general.
A study co-authored by Dr Katharine Smith and Professor Andrea Cipriani, with colleagues from King’s College London, the University of Toronto and Università degli Studi di Milano, explored the impact of COVID-19 on perinatal mental health in particular.
The study noted how the under-diagnosis and under-treatment of perinatal mental health issues have been magnified by the pandemic, highlighting the advantages of tele-psychiatry in a time of social restricted social contact, and raising the need for greater guidance and planning across organisations including government departments, health care providers, and the voluntary sector.
Parenting in crisis contexts.

Creating resources for parents in crisis settings.
Researchers from Oxford’s Department of Social Policy and Intervention are producing resources for parents to support the mental health of children in crisis contexts.
Professor Lucie Cluver and Dr Jamie Lachman lead the award-winning Parenting for Lifelong Health (PLH) initiative, developed in collaboration with the World Health Organisation (WHO), UNICEF, the United Nations High Commissioner for Refugees (UNHCR) and the United Nations Office on Drugs and Crime (UNODC), as well as academic colleagues from South Africa and the United Kingdom.
4 million +
families reached in Pakistan
Parenting for Lifelong Health, developed and tested by Dr Jamie Lachman, Professor Lucie Cluver, and Professor Frances Gardner, along with other UN and academic colleagues, is a suite of open access, non-commercialised programmes with a key goal of preventing child maltreatment and involvement in other forms of violence.
It also shows benefits in improving parent-child relationships, enhancing security of child attachment, and of child cognitive and socio-emotional development, reducing family mental health distress, increasing family economic resilience, and reducing substance use.
Evidence shows that preventing child maltreatment and later violence can also result in important long-term physical and mental health and socio-occupational benefits as children become adults and parents themselves.
The programmes are currently being delivered in 40 low- and middle-income countries across Sub-Saharan Africa, South-eastern Europe, Southeast Asia, and the Caribbean.
11.6 million +
families reached in Ukraine
This project has evolved into the Global Parenting Initiative led by Dr Lachman, which is testing hybrid and digital delivery approaches to support evidence-based parenting at scale.
Professor Cluver and Dr Isang Awah were among a group of Oxford experts who worked with Oxford University’s Ukrainian community to create a package of free, easy-to-use advice for families affected by the war.
‘These will help families to cope with stress, make safety plans for their children, support children through fear and danger, and build children’s resilience to crisis’
2023 earthquakes in Turkey and Syria.
The collegiate University offers its deepest sympathy and support to any student or staff member affected by the tragic events in Turkey and Syria.
On Thursday 9 February 2023, the Pro-Vice-Chancellor for People & Digital and the Pro-Vice-Chancellor for Education wrote to all University staff and students with Turkish or Syrian nationality offering support and practical advice.
Information, advice and support for staff and students impacted
Having reached over 15 million families in Ukraine and Pakistan, the Parenting for Lifelong Health team, led by Professor Cluver, Dr Lachman and Dr Awah, have again worked with the WHO, UNICEF, UNHCR and UNODC to create rapidly shareable social media assets and resources.
Based on 15 Oxford-University led randomised control trials of parenting interventions, the assets and resources include invaluable tips for parents and caregivers in Turkey and Syria.
Advice for parents and caregivers in Turkey and Syria.
More from PULSE.